The ectopia cordis is a disease rare that is defined by an abnormal position of the heart outside the thorax. Associated with parietal pericardium defectsdiaphragm, sternum and, in most cases, heart disease.
Theoretical aspects of ectopia cordis
The nomination of ectopia cordis it was first proposed by Abbott in 18981, although patients with similar defects had been described in previous decades under other names.
Byron classified the ectopia cordis in 4 groups: cervical, thoracic, thoracoabdominal, and abdominal. This last group includes patients with abdominal midline involvement (omphalocele) who meet the defining characteristics of the disease.
In 1958, Cantrell published a syndrome with 5 defects: abnormalities of the chest wall, abdominal, diaphragm, pericardium and heart.
CASE 1
We present a case of ectopia cordis in a preterm newborn (36 weeks), by eutocic vaginal delivery, which was uneventful.
This is a neonate with a thoracoabdominal wall defect. In the lower sternal region protrudes the covered cardiac tip by skin tissue and a supraumbilical hernia.
An echocardiogram is performed to rule out congenital heart disease and an MRI confirms the diagnosis of thoracoabdominal ectopia cordis. With midline defect of the lower anterior chest wall, herniation of the apex, small diaphragmatic defect in the insertion with the sternum and supraumbilical defect through which the apex is partially herniated. right hepatic lobe.
At 6 days of life surgically repairs, the heart is placed in the intrathoracic position, the umbilical vein is ligated and the adhesions to the wall of the right hepatic lobe are released. The evolution is satisfactory.
Ectopia cordis is a rare defect, with a incidence of 5.5–7.9 cases per million live births, in which the heart is exposed, totally or partially, in the thorax.
They are classified as cervical, thoracic, thoracoabdominal and abdominal. More than 80% of affected fetuses associated heart disease (usually the thoracoabdominal and thoracic forms). What ventricular septal defect, Tetralogy of Fallot, left ventricular diverticulum, double right ventricular outflow tract, and pulmonary hypoplasia. It represents 0.1% of congenital heart disease. It is a defect during embryogenesis, in which the fusion of the lateral folds in the thoracic area fails during the 6th postmenstrual week. This is one of the few cases that does not associate heart disease.
CASE 2
new born of 42 weeks gestation and birth weight of 2,900 g. At birth, the Following data: Apgar test 7 and 9 (5 min), cyanosis of skin and mucous membranes, polypnea with subcostal retractions. As well as omphalocele with open sternum and heart in the medial area.
The chest X-ray revealed absence of the diaphragm, with the abdominal viscera in the chest (incomplete thoracoabdominal ectopia cordis). The patient was operated, and died at 24 h. In the cardiac necropsy highlighted drainage of the superior and inferior vena cava in the right atrium and of the pulmonary veins in the left atrium, mitral atresia, perimembranous outflow ventricular septal defect, and emergence of the pulmonary artery and the aortic artery of the right ventricle.
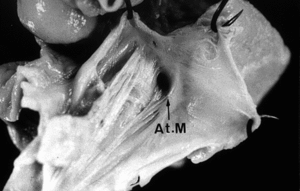
Furthermore, it was observed valve stenosis pulmonary and slight hypoplasia of the left ventricle. The coronary arteries arose from the anterior and left sinuses.
Related Notes:
Science advances! Hong Kong creates test to DETECT prolonged COVID-19
10 mistakes smart doctors make AVOID THEM!
Official Mexican NOM for the control of arterial hypertension


