5 minutes
Raynaud’s disease are episodes of decreased blood flow that cause discoloration of the skin. Why happens?
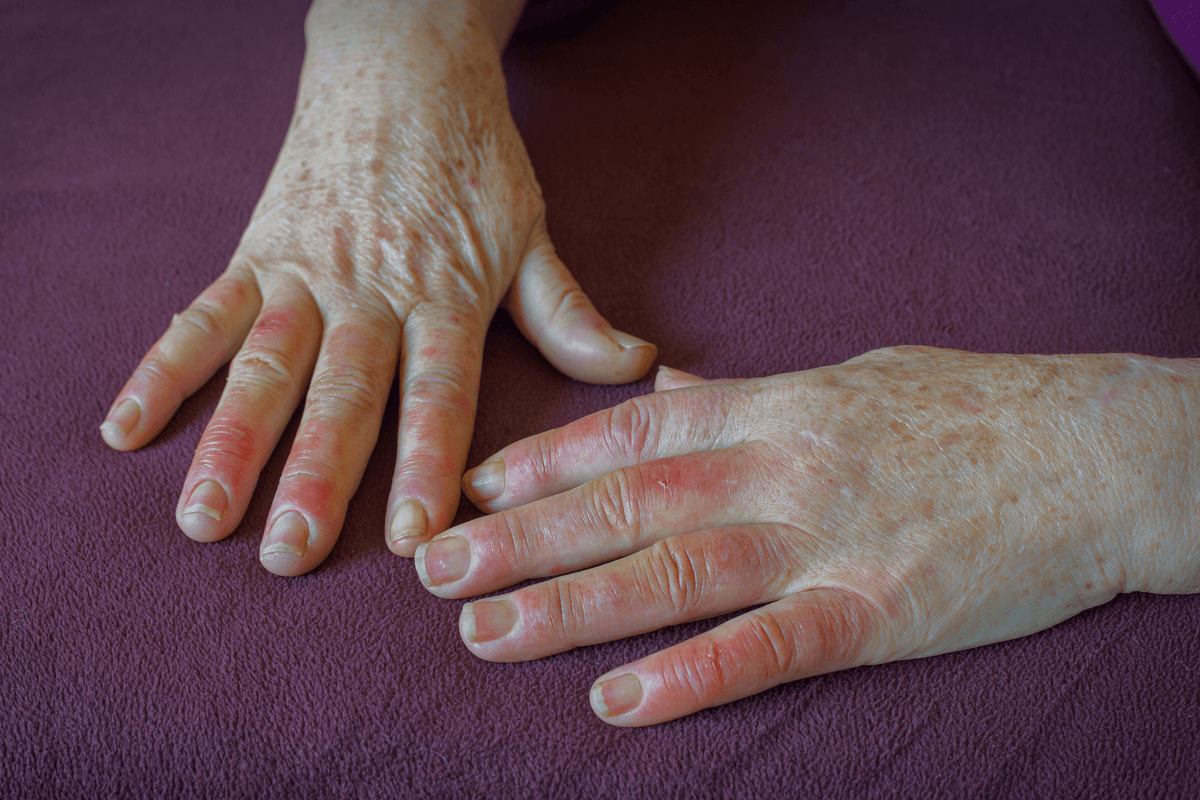
Raynaud’s disease is due to a temporary decrease in blood flow to the skin in response to specific stimuli such as stress or cold. Most commonly affects the fingers of the hands and then to the feet. In particular, these turn into three different colorations in response to stimuli.
Both its diagnosis and its treatment require the intervention of a specialist in rheumatology. The professional will evaluate the severity of the symptoms and determine if they are associated with another condition. Do you want to know more about it? Next, we inform you in detail.
What is Raynaud’s disease?
Raynaud’s disease is a condition that usually occurs in hypersensitive people. Specifically, it is produced by an exaggerated response of the blood vessels to factors such as emotional stress or cold. For now, no specific origin has been identified. Nevertheless, has a prevalence from 3 to 20% of the world population.
The first to describe this condition was Maurice Raynaud in 1862; hence its name. He defined it as a local lack of oxygen in the extremities due to an exaggerated response of the spinal cord on the blood vessels.
Symptoms
Simply put, Raynaud’s disease causes the following clinical manifestations:
- Cold extremities.
- Color changes in the skin (usually asymmetrical and respecting the thumbs in the case of the hands).
- Stabbing pain.
- Tingling and numbness
Another important factor is the episodic nature and associated with triggers, which is why it is more common during winter. Often, the limbs tend to take three different colorations due to constriction of blood vessels.
- The rapid and exaggerated decrease the skin turns pale and cold in color.
- When the decrease in blood flow is prolonged and there is oxygen deficiency in the tissues, they turn blue or cyanotic in color, and they feel numb.
- Once the blood flow is restarted, the influx of blood is rapid and exaggerated; therefore, it takes on a red or erythematous coloration. At this time palpitations, pricking pain, or swelling are usually felt.
There are some cases where the skin just turns pale. When this circumstance is prolonged, it can generate numbness, a feeling of heaviness and pain.
And while it predominates in the fingers and toes, it also tends to affect the ears, nose, face, nipples, and knee. It can even be manifested with livedo reticularis (patchy reddish and bluish discoloration on the skin) elsewhere.
All the symptoms are reversible when heating the zone or diminishing the stimulus; furthermore, they are transitory. However, when an artery is completely occluded for a long time, it can cause skin ulcers whose treatment requires the removal of the affected tissue.
Predisposing factors
- Female gender
- Age (more frequent between 15 and 40 years).
- Family background.
- Any underlying condition that affects the blood vessels.
- Living in cold climates (symptoms tend to be worse in winter and better in summer).
Is Raynaud’s syndrome the same as Raynaud’s phenomenon and Raynaud’s disease?
Raynaud’s phenomenon can be classified as primary or secondary. The primary is the so-called “Raynaud’s phenomenon” or “Raynaud’s disease.” Meanwhile, the term “Raynaud’s syndrome” is reserved for secondary Raynaud’s phenomenon.
Raynaud’s disease is one in which no other associated condition is identified that can cause it. It is more common in females, in those under 30 years of age and with a family history. It is usually bilateral, symmetrical and with little tendency to the formation of ulcers.
Raynaud’s syndrome is one in which there is an underlying condition that acts as a trigger. It usually appears at a later age, with asymmetric episodes, altered laboratories and in males. In particular, the pathologies associated with its appearance are the following:
- Connective tissue diseases, such as scleroderma or lupus erythematosus.
- Diseases such as atherosclerosis (hardening of the blood vessels due to the accumulation of cholesterol) and other cardiovascular diseases.
- Mellitus diabetes.
- Medicines such as beta blockers (bisoprolol) or migraine headaches (ergotamine and sumatriptan).
Raynaud’s disease diagnosis
To differentiate a primary case from a secondary Raynaud case, a test called “periungual capillaroscopy” is performed. With a microscope or magnifying glass, in this the blood vessels of the skin at the base of the nail are observed in search of alterations.
In cases of primary Raynaud’s disease, capillaroscopy is negative. In addition, in these cases the immunological tests and inflammatory markers are normal. Artery disease and other conditions that can cause decreased blood flow should be ruled out.
To determine if there is blockage of the arteries, a Doppler ultrasound may be performed before and after exposure to cold.
Raynaud’s disease treatment and prognosis
In mild Raynaud’s disease, treatment is to prevent exposure to the triggering agent. Therefore, it can be controlled by protecting areas that are susceptible to cold, such as the head, trunk, arms, hands and legs. Similarly, you can soak your hands in warm water when the attacks happen.
In addition, make some lifestyle modifications to maintain a suitable temperature and improve blood vessel circulation. To do this, it is recommended to do physical exercise, reduce exposure to stress and avoid the intake of tobacco and caffeine.
If medications are required, the doctor may suggest agents that dilate the blood vessels, such as the following:
- Alpha adrenergic blockers (dibenziline).
- Calcium channel blockers (amlodipine, nifedipine).
- Angiotensin receptor blockers (prazosin).
The prognosis for Raynaud’s disease is good. Although the symptoms may be bothersome at the moment, they are not disabling and can be controlled.
It might interest you …